Mad Woman
A controlling, philandering husband. A string of tragic losses. A life spent in isolation. This isn’t the plot of Reese Witherspoon’s next miniseries; it’s the regrettably true story of Juana of Castile, as told by Stefanie last week. Juana is known to history as “Juana the Mad”. The charges against her? Attacking her husband’s mistress, excessively grieving over his death, and going through fits of “hysteria” where she would refuse to eat, sleep or talk until she got her way.

When you consider the fact that she was mistreated in her marriage, thrust into a position of power that she never anticipated to have, and used as a pawn by the people who loved her most, her behavior does not seem so mad. In addition, the portrayal of Juana as mentally unstable was leveraged to keep her from ruling over a unified Spain, so must be evaluated with a critical eye.
Even so, I think it’s safe to say that Juana was more than just sad. While Isabella of Castile had high hopes that her daughter would embody the strong, educated female leader that she had tried to raise, Juana unfortunately ended up colored by the same depression that afflicted her mother and grandmother. The question is: if depression was an appropriate response to the cards that life dealt her, can it truly be considered pathological?
Misery Business
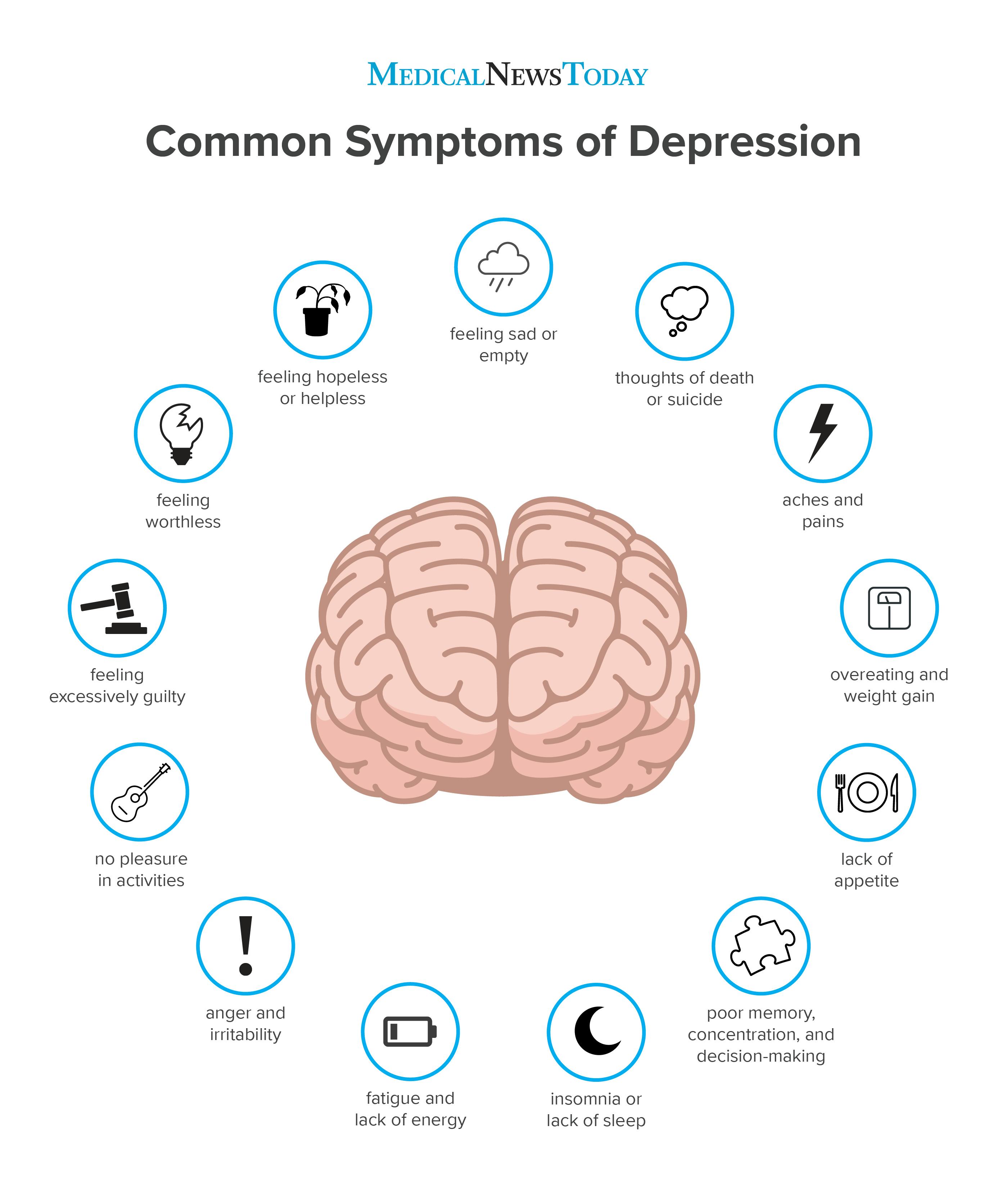
To receive a diagnosis of depression, also known as Major Depressive Disorder (MDD), under the DSM-5, a person must have experienced symptoms for at least two weeks that interfere with their daily functioning and aren’t explained by a medication or other psychiatric disorder. Diagnosis requires the presence of at least five symptoms, one of which must be depressed mood or reduced interest or pleasure in activities. Other symptoms include low energy, inability to concentrate, feelings of guilt or worthlessness, self-perceived slowed thoughts or movements, and unintentional changes in weight or appetite. In the most serious cases, patients have recurring thoughts of suicide. As you can appreciate, depression is not the same as sadness. Depression has physical, emotional, and mental effects and impairs an individual’s ability to function. Note that there are other forms of depression, like dysthymia, postpartum, and seasonal, but we will focus on MDD as it is the most common.
In the US alone, 7.1% of all adults experienced at least one episode (at least two weeks) of MDD in 2017. Shockingly, over 13% of teens 12-17 had a depressive event in the same year. More females were affected in both age groups.
Juana’s mental instability was certainly exaggerated for political and financial gain on the part of her husband, father, and son. Likewise, it seems like some of Juana’s extreme behavior was a cry for attention or an attempt to manipulate those who held power over her. However, there were signs that she was legitimately suffering from MDD. One source who saw her after Philip left her alone for the birth of their son described the “‘disposition of the lady princess…such that it should greatly pain not only those so affected and who love her so, but even strangers, because she sleeps poorly, eats little, and sometimes nothing. She is very sad and quite thin’” (Tremlet). We can check off low energy, depressed mood, and changes in appetite. There is also no evidence that Juana ever experienced any symptoms like mania or hallucinations that would indicate she was suffering from a different disorder in which depression is a symptom. And since big pharma wasn’t exactly booming in the 15th century, it’s safe to say that her mood changes weren’t the side effect of a medication. In sum, it seems reasonable to conclude that Juana of Castile was not mad; she was depressed.
Neurotransmission Impossible
If you haven’t yet sensed a theme here at ULTC, it’s that mental illness is the result of genetic and environmental factors. In this house, we acknowledge nature and nurture. MDD is no exception to this rule. Studies estimate that about half of a person’s risk of developing depression is genetic, and that people who have a genetic predisposition still require an environmental trigger before displaying symptoms. These triggers are usually stressful events, like being cheated on, losing a loved one, or being locked in isolation by your family so that they can take your throne…just to name a few.
Normally, when a treatment is developed for a disease, scientists first seek to understand the biology underlying it. That helps them figure out what molecules, cells, or proteins their drug should target. The process was completely inverted for depression treatment. By chance, it was observed that a couple of drugs improved depression symptoms. Then scientists worked backwards to figure out what the mechanism of the medication was, and thus what was going on in a depressed person’s brain.
If you remember from a previous post, the synapse is the junction between neurons where they can communicate in the form of chemicals called neurotransmitters. Scientists found that drugs that improved depression symptoms allowed neurotransmitters to stay in the synapse longer. Specifically, preventing the clearance of serotonin and norepinephrine from the synapse improved depression symptoms. This suggested that there was reduced serotonin and norepinephrine signaling during depression, and boosting their activity by letting them hang around in the synapse could be therapeutic.
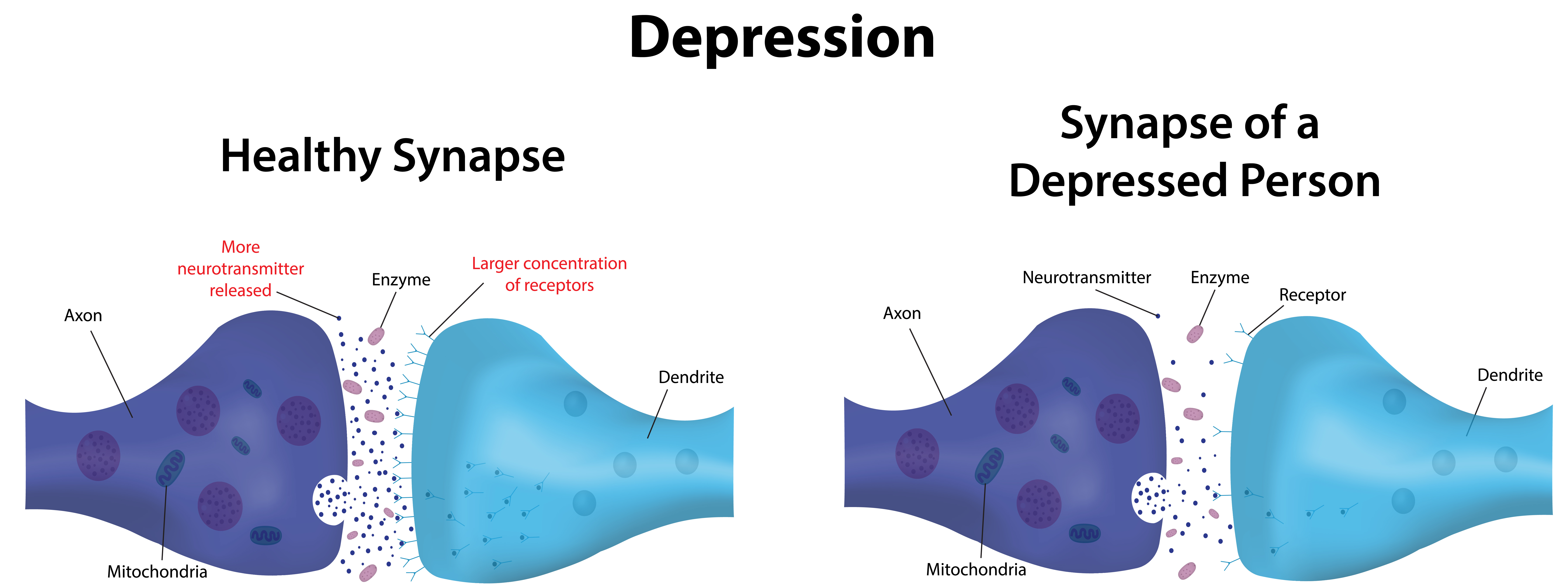
In popular science, serotonin is known as the neurotransmitter that makes you happy, and norepinephrine is the one that makes you feel aroused and alert, so it would make sense that they have reduced functioning in depression. But serotonin and norepinephrine play roles in many brain regions and have diverse functions. Disturbances to their signaling results in complex symptoms that are difficult to target clinically. However, it should be noted that it’s still unclear if reduced serotonin and norepinephrine signaling drive depression or are a symptom of the disease. In addition, other biological mechanisms have been implicated in MDD pathogenesis, but I don’t have time to go into them all here.
Brain regions that have been implicated in MDD include the hypothalamus, which has roles in sleep and feeding, the amygdala, which contributes to fear and anxiety, the striatum, which supports emotional memory and pleasure, and the cortex, which is involved in executive functioning. All of these functions are affected by MDD, suggesting that the widespread clinical manifestations of depression are reflected by widespread alterations in brain activity.
Circumstantial Evidence
I outlined the diagnosis criteria for MDD in the DSM-5 bit earlier. What I failed to mention was that there was a good deal of controversy over the changes made in this edition. In previous versions of the DSM, a diagnosis could not be made if the patient was grieving. However, in the fifth edition, this bereavement clause was removed, meaning that even if someone was grieving the loss of a loved one, or dealing with a circumstance like a lost job that could explain their depressive symptoms, they could still be given a diagnosis of MDD. There were some legitimate reasons for removing this exclusion criteria. Psychologists argue that there is a difference between normal grieving and depression caused by grieving that has a debilitating effect on a person’s ability to function. In addition, the change highlights the fact that grief can be a stressor that triggers MDD development, and therefore should be addressed clinically.
However, it also blurs the lines between pathological and normal responses to life events. There is no one way to grieve. While some people thought Juana’s reaction to Philip’s death was over the top, it could have been an appropriate way for her to process the emotions of her complicated loss. The point that clinicians are trying to make is that even when a depressive response is understandable given the circumstances, changes in mood that alter your ability to function in social and professional environments are not normal. Because the stakes are so high with MDD due to the high risk of suicides, even a depression that seems understandable is one that should be addressed. It can therefore be argued that although Juana’s reactions to her husband’s infidelity or her grief over Philip’s death were seemingly justifiable, they were still ultimately harmful.
Gut Feeling
Because I want you to be up to date on all the latest in neuroscience, I want to take a moment before signing off to tell you what’s hot right now in depression research: the gut. The brain is constantly in contact with the gut in order to control things like digestion, but about 15 years ago, researchers found that the gut can talk back. The gut is populated by a swarm of micro-organisms that can have positive or negative effects on your body. Interestingly, these microbes in the digestive system make up to 90% of the body’s serotonin, which hinted to scientists that they may be involved in MDD development or progression.
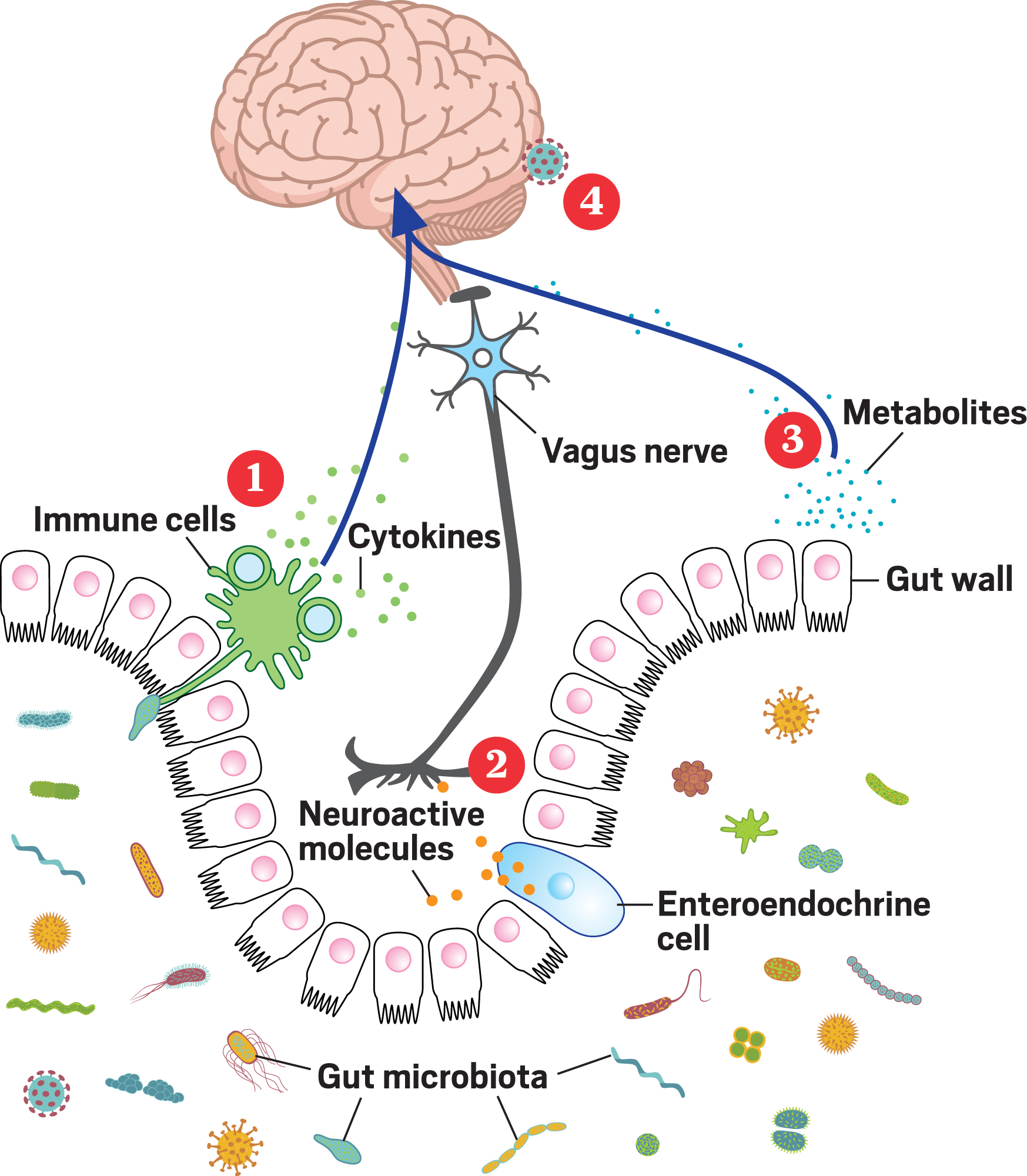
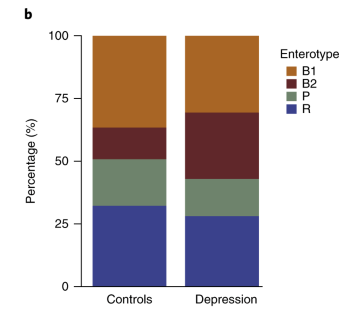
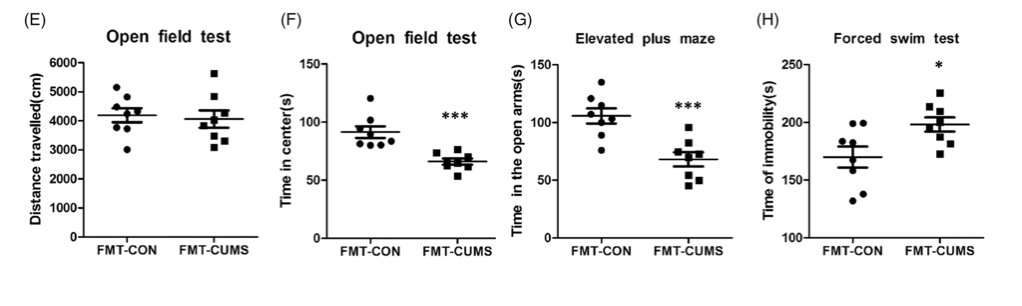
A 2019 study that characterized the gut microbiomes of over 1,000 Finnish individuals showed that the abundance of specific microorganism species differed between depressed and healthy individuals. Another study from last year depleted the microbiome of mice using antibiotics and then performed a fecal transplant from normal or chronically stressed mice. Mice who received a fecal transplant from a chronically stressed mouse had higher levels of anxiety and depression-like behavior. This suggests that stress and the microbiome have reciprocal effects on one another, and could be driving symptoms of depression.
A biotech start up is now leveraging this research to develop a treatment for psychiatric disorders including depression using neurotransmitter-producing bacteria, the human-palatable equivalent to the mouse fecal transplants. The gut-brain axis is also a focus of research for diseases like Autism and Parkinson’s, reflecting the intimate connection between the brain and the environment, and offering an exciting path forward for future research.
Double-Edged Sword
Juana’s mental illness was used as evidence that she was unfit to rule. But depression isn’t like some of the other disorders we have talked about in which a person has no control of their behavior or a distorted perception of reality. In psychological terms, Juana didn’t experience psychosis, and in colloquial terms, she wasn’t insane. She was capable of ruling her kingdom.
In fact, many great world leaders have suffered from depression throughout history. Dr. Nassir Ghaemi is a psychiatrist at Tufts University who uses historical and medical records to identify mental illness in historical figures (way to steal our thunder…). He has proposed that Winston Churchill and Martin Luther King Jr. are some examples of great leaders who suffered from depression. And they definitely didn’t seem unfit to rule!
Interestingly, a classic 1979 study suggested that depressed individuals may have a more accurate sense of reality, a line of questioning that psychologists have continued to pursue. In addition, there is a complicated body of research aiming to determine if mood disorders are more prevalent in creative individuals. Although the literature on these traits in depressed individuals isn’t entirely conclusive, I think they shed light on the important truth that people suffering from depression have things to offer the world. Juana of Castile certainly did, but never got the opportunity to share her gifts. Next week, Stefanie will tell us how her isolation ultimately made its mark on history.
If you or someone you know is struggling with depression or suicidal ideation, call the Suicide Prevention Lifeline at 1-800-273-8255.
References
Alloy, L. B., & Abramson, L. Y. (1979). Judgment of contingency in depressed and nondepressed students: Sadder but wiser? Journal of Experimental Psychology: General,108(4), 441-485. doi:10.1037/0096-3445.108.4.44
Borenstein, S. (2016, August 11). Some great leaders had mental illness – it may have helped. Retrieved from https://medicalxpress.com/news/2016-08-great-leaders-mental-illness-.html
Kavan, M. G., & Barone, E. J. (2014, November 15). Grief and Major Depression-Controversy Over Changes in DSM-5 Diagnostic Criteria. Retrieved from https://www.aafp.org/afp/2014/1115/p690.html
Li, N., Wang, Q., Wang, Y., Sun, A., Lin, Y., Jin, Y., & Li, X. (2019). Fecal microbiota transplantation from chronic unpredictable mild stress mice donors affects anxiety-like and depression-like behavior in recipient mice via the gut microbiota-inflammation-brain axis. Stress,22(5), 592-602. doi:10.1080/10253890.2019.1617267
Major Depression. (n.d.). Retrieved from https://www.nimh.nih.gov/health/statistics/major-depression.shtml
Nestler, E. J., Barrot, M., DiLeone, R. J., Eisch, A. J., Gold, S. J., & Monteggia, L. M. (2002, April 04). Neurobiology of Depression. Retrieved from https://www.sciencedirect.com/science/article/pii/S0896627302006530
Pennisi, E. (2020, May 11). Meet the ‘psychobiome’: The gut bacteria that may alter how you think, feel, and act. Retrieved from https://www.sciencemag.org/news/2020/05/meet-psychobiome-gut-bacteria-may-alter-how-you-think-feel-and-act
Taylor, C. L. (2017). Creativity and Mood Disorder: A Systematic Review and Meta-Analysis. Perspectives on Psychological Science,12(6), 1040-1076. doi:10.1177/1745691617699653
Truschel, J. (2020, September 25). Depression Definition and DSM-5 Diagnostic Criteria. Retrieved from https://www.psycom.net/depression-definition-dsm-5-diagnostic-criteria/
Valles-Colomer M;Falony G;Darzi Y;Tigchelaar EF;Wang J;Tito RY;Schiweck C;Kurilshikov A;Joossens M;Wijmenga C;Claes S;Van Oudenhove L;Zhernakova A;Vieira-Silva S;Raes J;. (n.d.). The neuroactive potential of the human gut microbiota in quality of life and depression. Retrieved from https://pubmed.ncbi.nlm.nih.gov/30718848/
Yano, J., Yu, K., Donaldson, G., Shastri, G., Ann, P., Ma, L., . . . Hsiao, E. (2015). Indigenous Bacteria from the Gut Microbiota Regulate Host Serotonin Biosynthesis. Cell,161(2), 264-276. doi:10.1016/j.cell.2015.02.047


Very informative. This has put a lot if things in perspective for me.
LikeLike